Receiving an Abnormal Mammogram Report, What Next?
It is not unusual to get recalled after an initial screening mammogram. Additional imaging is often requested so that a clearer view of a particular area of breast tissue can be captured. Fewer than one in 10 women who return for additional testing are found to have cancer.
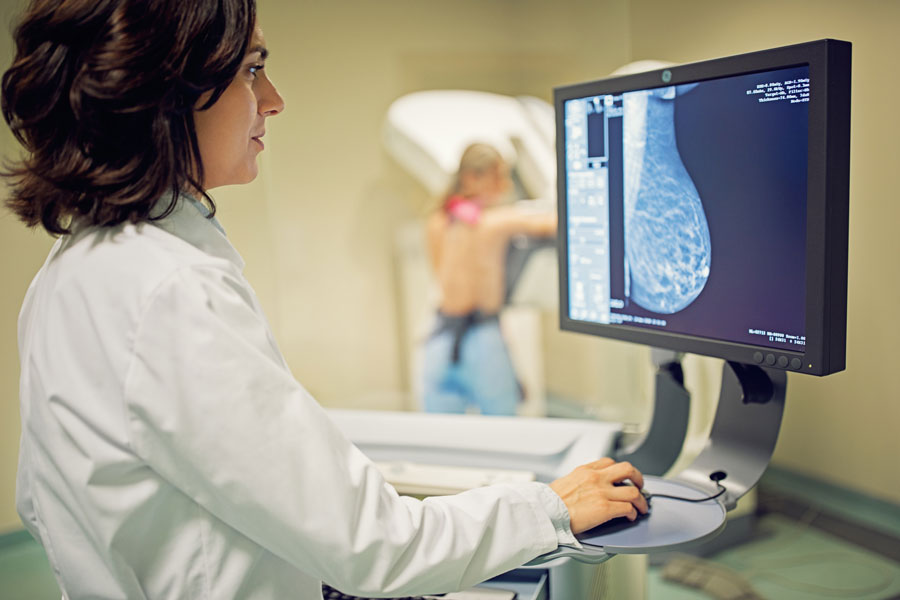
Here are a few reasons your radiologist may call you back:
- The first images were unclear or missed some part of your breast tissue
- There is an area that looks different from other parts of your breast
- The appearance of a suspicious-looking mass or calcifications
Quite often, when the area in question is compressed and more closely scrutinized, it is no longer suspicious looking and is not found to be cancerous.
“Additional testing may cause patients to worry,” said Dr. Lindsey Beakley, breast surgical oncologist at Southern Cancer Center. “But many times, follow-up requests are the checks and balances needed to verify that findings are benign. And if there is a concerning finding, we can address it as soon as possible.”
What Do the Results Mean?
It helps to understand how doctors report results. Doctors use the Breast Imaging Reporting and Data System (BI-RADS) to describe what is found on a mammogram. Categories run from zero to six and help doctors use a common language to describe and categorize their findings:
Category 0: Incomplete. Additional imaging or previous imaging tests are needed because the radiologist needs clarification. Another mammogram with spot compression, different views, or an ultrasound may be requested.
Category 1: Negative. Nothing new or abnormal was found. Breasts are symmetrical with no masses, abnormal structures, or suspicious calcifications.
Calcifications are small deposits of calcium seen but not felt in the breast tissue. They are not the result of diet or supplements. They are a byproduct of breast cell growth and division. There are two types:
Microcalcifications: Tiny calcifications that may require additional testing. They can become cancerous.
Macrocalcifications: Larger, coarser areas of calcium commonly found in women 50+ years, which can be the natural result of aging, past breast injury, or buildup, such as calcium oxalate, that occurs over time.
Category 2: Benign or non-cancerous finding. This is also a negative test. However, the radiologist records and describes benign calcifications, masses, lymph nodes, or any changes from prior procedures so that other doctors can correctly read the mammogram.
Category 3: Probably benign. Follow-up within a shortened time frame is suggested. A finding in this category has no more than a two percent chance of being cancer. It is not expected to change over time but can’t definitively be labeled as benign. Repeat imaging within six to 12 months and regularly thereafter is recommended until the finding is determined to be stable, usually over a period of two years. Consistent screening allows for early diagnosis and intervention if significant changes occur.
Category 4: Suspicious or abnormal finding. It may not be cancer but could be. A surgical biopsy (removal of a small sample of breast tissue) is recommended. There are three subcategories:
- 4A: Low likelihood of cancer (between two and 10% chance)
- 4B: Moderate likelihood of cancer (more than a 10% chance, but not more than 50%)
- 4C: High likelihood of cancer (more than a 50% chance, but less than 95%)
Category 5: Highly suggestive of a malignancy. The finding looks like cancer and has at least a 95% chance of being cancer. A biopsy is very strongly recommended.
Category 6: Known malignancy proven by biopsy. This category is only used for a finding already determined to be cancerous. At this category level, imaging is used to monitor the patient’s response to treatment.
What Happens at the Follow-Up?
If you are recalled, the next step typically involves another mammogram, called a diagnostic mammogram. Your radiologist will direct the tech to take specific pictures of your breast and ensure all necessary views are captured. You may also receive a breast ultrasound, which uses sound waves to get additional images, or a breast MRI (magnetic resonance imaging) which uses radio waves and magnets to create an even more detailed picture. MRIs can detect small changes that are not always visible in mammograms or ultrasound.
If the area is still thought to be suspicious, a biopsy will be performed. Even if a biopsy is recommended, it does not automatically suggest that you have cancer. In fact, most results turn out to be benign, but biopsy and analysis are the only way to be sure.
What Else Should I Know?
Breast Density
Dense breasts are common, and almost half of all women 40+ years have them.
Dense breast tissue has a high composition of glandular and fibrous connective tissue and a relatively low percentage of fatty tissue, which can make mammograms more difficult to interpret. Women with dense breasts may be asked to return for follow-up testing more often than women with fatty breasts.
There are four BI-RADS breast density categories:
- Category A: Least dense
- Category B: Scattered areas of dense tissue
- Category C: More density (heterogeneous density)
- Category D: Extremely dense
If your breast tissues are in Category C or D, ask your doctor about whether additional testing is recommended.
Testing Recommendations
Mammograms use only small doses of radiation. The risk of harm is low, but repeated mammograms can potentially increase cancer risk. Always speak with your doctor about what is suitable for you, particularly if there is any possibility of a pregnancy.
High-risk women should have an annual mammogram, which may be supplemented with additional screenings, such as an MRI.
What Next?
Waiting for results can be unnerving, but most often, follow-tests show normal tissue or a benign condition. Talking with loved ones or other women who have had screenings or biopsies can be helpful. And always speak with your doctor if you have any questions about your findings or test recommendations.
Sources:
Mammogram Results | Understanding Your Mammogram Report (cancer.org)
Breast Calcifications: Causes, Types, Biopsy and More (cancercenter.com)
Getting Called Back After a Mammogram | Mammogram Call Back (cancer.org)
Dense Breasts: Answers to Commonly Asked Questions – NCI (cancer.gov)
